The laparoscopic liver resections—an initial experience and the literature review
In general, liver surgery has seen significant advances in the last decades, particularly associated with improvements in anesthesia and critical care as well as surgical techniques. The improved understanding of the vascular anatomy of the liver based on Couinaud segments, has also led to a great reduction in morbidity and mortality associated with liver resection (1).
Clearly challenging, the laparoscopic liver resections (LLRs) were not accepted until recently due to the several reasons: the problem of intraoperative bleeding control, the technical difficulties, the learning curve and the fear of gas embolism (2). Since the first reported cases of liver resection in 1991 and 1992 (3,4), more than 3,000 cases have been reported in literature worldwide.
In general, LLR is associated with significant advantages: faster recovery, less post-operative pain, less morbidity, easier subsequent surgery and better cosmetic results (5). At first the indications limited to easily accessible tumors mostly placed at the peripheral portion of liver, the anterolateral segments (II, III, V, VI and the inferior part of IV liver segment) (6,7). The majority of initial reports suggested that LLR is poorly indicated when the lesion is located in the posterior or superior part of the liver (segments I, VII and VIII, the same as the superior part of segment IV) (8,9).
The indications for LLRs widened from solitary, small, easily approachable lesions, to more demanding procedures including the major liver resections such as left and right hepatectomies (10-14). The disease-related indications for LLRs included various conditions of benign, but also the malignant diseases especially the hepatocellular carcinoma and colorectal liver metastases (15-21).
In our department the laparoscopic surgical procedures are widespread. The laparoscopic cholecystectomies and appendectomies are performed routinely and have outnumbered the open cholecystectomies and appendectomies that are done only in a narrow spectrum of indications. Apart from that the explorations, the ulcer perforation and hernia repair are performed laparoscopically, as well. During last 10 years the elective splenectomies and colon resections are performed laparoscopically in the high number of cases.
On the other hand, more than 100 open liver resections are performed per year. The experience in laparoscopic surgery and open liver surgery encouraged our surgeons to start performing LLRs. There have already been some reports of laparoscopic operations of the echinococcic cysts performed in our institution (1,10,11).
Through this paper we aim to report our initial experience in laparoscopic liver surgery with the emphasis on the first left lateral bisegmentectomy and to show a brief literature review onto the main problems and concems concerning the LLRs.
Report of a case
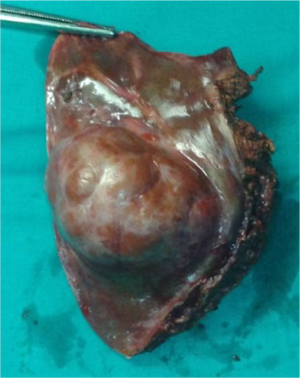
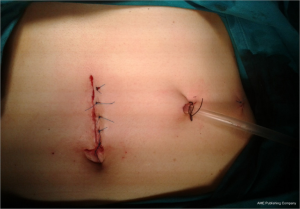
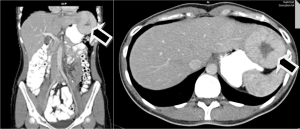
A 29 years old female patient was admitted to hospital for operative therapy of a liver tumor found on a magnetic resonance imaging (MRI) scan preformed as gastroenterological workup for symptoms related to chronic gastritis (Figure 1). There were no co-morbidities other than mild ankylosing spondylitis and the general clinical state was proper to the age of the patient. According to MRI record the tumor was situated at the left hepatic lobe and its diameters were 62×57 mm. There were no other tumors found inside of the abdominal and thoracic cavity. The patient underwent the laparoscopic left lateral bisegmentectomy of the 2nd and 3rd liver segments (Figure 2). The resection was performed throe three skin incisions (Figure 3), using the harmonic scalpel and the vascular structures were ligated by the endoscopic vascular staplers (35 and 45 mm). The operation lasted for an hour. The patient spent a day in intensive care unit (ICU). There were no any early complication found and the patient was released home on the third postoperative day. The pathology of the resected tumor had shown the follicular nodular hyperplasia. The consequent perioperative period passed without complications.
Report of laparoscopically treated patients with echinococcic liver disease
In our institution 15 laparoscopic pericistectomies were performed to date. All patients were pre-operatively treated with albendazole. Total pericystectomy without opening the cyst cavity was performed laparoscopically in seven patients, while the partials pericystectomy was done laparoscopically five patients. In another three patients the procedure started laparoscopically but were converted and completed as an open procedure. The median operative time was 67.5 minutes (range, 60.0-120.0 minutes) and the median hospital stay 5.0 days (range, 4.0-7.0 days). In one patient the echinococcic cyst was situated in 7th liver segment and another three cysts were found intraabdominaly. All of them were removed laparoscopically. There were no complication nor recurrences reported until now in laparoscopically operated patients. During the same period of time 32 patients underwent the open operation of the echinococcic liver cysts. In those patients the operation lasted longer [mean operative time 100.0 minutes (range, 60.0-210.0 minutes)]. On the other hand, the hospital stay was longer in patient that underwent the open surgical procedure [median hospital stay 8.0 days (range, 7.0-14.0 days)]. Also there was one case of recurrence in patient treated with the open procedure 3 years following the operation. There was no mortality reported until now in both groups of patients.
Discussion
As the experience and technical improvement grow the spectrum of indications expands. According to recently published study the LLR can be performed safely in selected patients with both benign and malignant liver tumors regardless to the dimensions, location or previous operating history with comparable morbidity and mortality to those in open surgical procedures (12). LLRs were concluded to be comparable or even better than open liver resection in the context of intraoperative blood loss and the length of hospital stay (13). A similar or lower mortality (0.3%) and morbidity (10.5%) were reported at LLR in comparison to open operative technique of the liver resection (14). There was no significant difference in overall and disease-free 5-year survival rate for hepatocellular carcinoma between open and laparoscopic hepatectomies (15). The conversion rates vary from 8.1% to 17.6% and the reported rate of complications was 3.6% with the postoperative bile leakage rate of 1.1% in 27 analyzed studies that included 619 patients (16).
Conclusions
In our initial experience of operated patients the performed laparoscopic surgical procedures were found safe and efficient with the acceptable operative time and hospital stay. The data found in literature are encouraging, however the proper surgical training and experience the same as well technically equipped centers are essential for performing LLRs.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Busić Z, Lemac D, Stipancić I, et al. Surgical treatment of liver echinococcosis--the role of laparoscopy. Acta Chir Belg 2006;106:688-91. [PubMed]
- Cai X, Li Z, Zhang Y, et al. Laparoscopic liver resection and the learning curve: a 14-year, single-center experience. Surg Endosc 2014;28:1334-41. [PubMed]
- Reich H, McGlynn F, DeCaprio J, et al. Laparoscopic excision of benign liver lesions. Obstet Gynecol 1991;78:956-8. [PubMed]
- Gagner M, Rheault M, Dubuc J. Laparoscopic partial hepatectomy for liver tumor Surg Endosc 1992;6:99.
- Tranchart H, Dagher I. Laparoscopic liver resection: a review. J Visc Surg 2014;151:107-15. [PubMed]
- Gigot JF, Glineur D, Santiago Azagra J, et al. Laparoscopic liver resection for malignant liver tumors: preliminary results of a multicenter European study. Ann Surg 2002;236:90-7. [PubMed]
- Kaneko H, Takagi S, Shiba T. Laparoscopic partial hepatectomy and left lateral segmentectomy: technique and results of a clinical series. Surgery 1996;120:468-75. [PubMed]
- Laurent A, Cherqui D, Lesurtel M, et al. Laparoscopic liver resection for subcapsular hepatocellular carcinoma complicating chronic liver disease. Arch Surg 2003;138:763-9; discussion 769. [PubMed]
- Dulucq JL, Wintringer P, Stabilini C, et al. Laparoscopic liver resections: a single center experience. Surg Endosc 2005;19:886-91. [PubMed]
- Busić Z, Cupurdija K, Servis D, et al. Surgical treatment of liver echinococcosis--open or laparoscopic surgery? Coll Antropol 2012;36:1363-6. [PubMed]
- Busić Z, Lovrić Z, Kolovrat M, et al. Laparoscopic operation of hepatic hydatid cyst with intraabdominal dissemination--a case report and literature review. Coll Antropol 2009;33 Suppl 2:181-3.. [PubMed]
- Han HS, Yoon YS, Cho JY, et al. Laparoscopic liver resection for hepatocellular carcinoma: korean experiences. Liver Cancer 2013;2:25-30. [PubMed]
- Simillis C, Constantinides VA, Tekkis PP, et al. Laparoscopic versus open hepatic resections for benign and malignant neoplasms--a meta-analysis. Surgery 2007;141:203-11. [PubMed]
- Nguyen KT, Gamblin TC, Geller DA. World review of laparoscopic liver resection-2,804 patients. Ann Surg 2009;250:831-41. [PubMed]
- Kaneko H, Takagi S, Otsuka Y, et al. Laparoscopic liver resection of hepatocellular carcinoma. Am J Surg 2005;189:190-4. [PubMed]
- Laurence JM, Lam VW, Langcake ME, et al. Laparoscopic hepatectomy, a systematic review. ANZ J Surg 2007;77:948-53. [PubMed]
- Jurisić I, Paradzik MT, Jurić D, et al. National program of colorectal carcinoma early detection in Brod-Posavina County (east Croatia). Coll Antropol 2013;37:1223-7. [PubMed]
- Milas J, Samardzić S, Miskulin M. Neoplasms (C00-D48) in Osijek-Baranja County from 2001 to 2006, Croatia. Coll Antropol 2013;37:1209-22. [PubMed]
- Samardzić S, Mihaljević S, Dmitrović B, et al. First six years of implementing colorectal cancer screening in the Osijek-Baranja County, Croatia--can we do better? Coll Antropol 2013;37:913-8. [PubMed]
- Boras Z, Kondza G, Sisljagić V, et al. Prognostic factors of local recurrence and survival after curative rectal cancer surgery: a single institution experience. Coll Antropol 2012;36:1355-61. [PubMed]
- Krebs B, Kozelj M, Potrc S. Rectal cancer treatment and survival--comparison of two 5-year time intervals. Coll Antropol 2012;36:419-23. [PubMed]