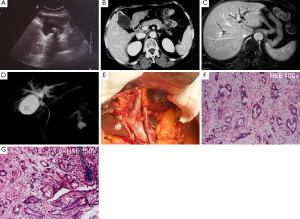
Double carcinomas simultaneously identified in biliary system
A 66-year-old female who had history of asymptomatic gallstone for three years was referred to our clinic because of a 14-day jaundice and dark-colored urine. Physical examination showed the liver being palpable under the right hypochondrium. Biochemistry assay showed alanine aminotransferase 87 U/L, total bilirubin 115.9 µmol/L, and direct bilirubin 93.8 µmol/L. Carcinoembryonic antigen (CEA) lever was within normal range, but carbohydrate 19-9 (CA19-9) lever was significant elevated (285.9 U/mL). Abdominal ultrosonography (US) exhibited a thickening gallbladder wall, and there were multiple strong echogenic focuses with acoustic within the gallbladder that moved with the change of patient’s position (Panel A). Portal vein was normal by Color Doppler flow imaging. Computed tomography (CT) revealed dilated intrahepatic biliary ducts, and delayed enhancement in gallbladder fundus, besides that both the caliber of common bile duct (CBD) and the size of gallbladder were normal (Panel B). Magnetic resonance imaging (MRI) showed an ill-defined lesion located in porta hepatis with iso-intense on T1-weighted images and slightly hyperintense on T2-weighted images, where poor enhancement was noted during the arterial phase, and a progressive increase of contrast enhancement was acquired in subsequent portal-venous and equilibrium phases (Panel C). Intrahepatic biliary duct was markedly dilated, and gallstones were observed as well. Dilatations of intrahepatic duct were found through magnetic resonance cholangiopancreatography (MRCP) with separate occlusions of the common hepatic duct (CHD), and left and right hepatic duct (Panel D). Hilar cholangiocarcinoma and gallstones were diagnosed, and laparotomy was performed under general anesthesia. Brownish green cholestasis and multiple gallstones with gallbladder fundus thickening were noted during the surgery. Right hepatic duct (RHD) markedly dilated to 2.0 cm in diameter. A mass could be touched within CHD and origin of left hepatic duct (Panel E). No dilatation of CBD was found. The resected gallbladder specimen was confirmed as an adenocarcinoma by intro-operative prompt pathology. Distant organ metastasis and peritoneal dissemination were not detected. Left hemihepatectomy (II, III, IV) with V segmentectomy, combined with excision of the entire extrahepatic biliary apparatus, along with a complete porta hepatis lymphadenectomy were finally performed. Biliary reconstruction was carried out by a RHD with Roux-en-Y cholangiojejunostomy. The histopathology of surgical specimen verified a moderately differentiated adenocarcinoma in gallbladder, which had invaded the whole gallbladder walls (Panel F), and a moderately or poorly differentiated adenocarcinoma of CHD (Panel G). The resected liver and the surgical margins of CBD and CHD were all free of lesions. The metastases in lymph nodes were demonstrated in group 3 and 5. However, the lymph nodular group 7, 8, 9 and 12 were negative. The pleural effusion was the main postoperative complication. The patient was discharged on the 23rd postoperative day.
Acknowledgements
Disclosure: The authors declare no conflict of interest.