Twenty-eight years of repeated relapse of gastrointestinal stromal tumor
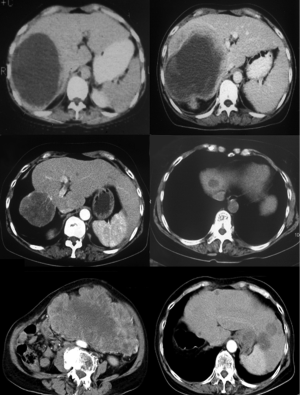
A 69-year-old female was admitted for treatment of an abdominal mass that was increasing in size. A 4-cm diameter abdominal mass was first noted 2 years previously. Over the past year, the mass gradually increased in size, but no associated gastrointestinal or systemic symptoms or signs were noted. Physical examination revealed an obvious lower abdominal bulge, with a palpable 20-cm diameter nontender mass. She had previously undergone subtotal gastrectomy for a gastrointestinal stromal tumor (GIST) of the stomach in 1985, resection of the right lobe of the liver and gallbladder for GIST metastasis in 1998, resection of metastatic lesions in the left lobe of the liver in 2003, and resection of metastatic GIST in the left lobe of the liver in 2007. Preoperative laboratory test results were unremarkable. Abdominal computed tomography showed a 20-cm diameter space-occupying mass in the abdominal cavity. Abnormal liver morphology was observed, with enlargement of the left caudate lobe and a 5-cm diameter lesion in the left lobe. The patient underwent resection of the huge abdominal metastatic GIST. Intraoperative exploration also revealed a palpable 4-cm diameter mass in the residual left hepatic lobe. The pathological diagnosis was GIST measuring 21 cm × 17 cm × 13 cm, with 15 mitoses per 50 high-power fields, indicating a high risk of recurrence. Radiofrequency ablation (RFA) of the left lobe metastasis was performed 7 days after surgery. Targeted therapy such as Gleevec was not administered. She developed multi-liver metastases afterwards, and was treated again by RFA. She died 20 months after the last surgery, that was 28 years after first stomach surgery for GIST.
Acknowledgements
Disclosure: The authors declare no conflict of interest.