Adenosquamous carcinoma arising in a duplication cyst of the gallbladder
A 52-year-old woman, previously healthy was admitted to another hospital due to right upper quadrant abdominal pain, fever and leukocytosis. An ultrasound demonstrated acute cholecystitis and lesion 8 cm. in diameter near the gallbladder. An abdominal CT scan showed the lesion in close proximity to the gallbladder, with fat infiltration. A percutaneous drainage of the lesion under CT guidance yielded a substance which was bloody and purulent in content. The patient improved clinically under antibiotics and was discharged from hospital with a recommendation for elective exploratory laparoscopy.
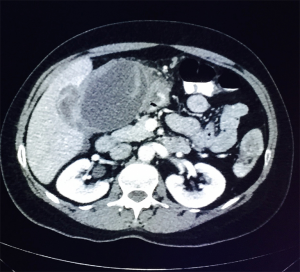
One month later, the patient was admitted to our hospital with high fever and right upper abdominal pain. An abdominal CT scan revealed a heterogeneous lesion, 19 cm × 9 cm × 7 cm. in size, with a differential diagnosis of hematoma, abscess or malignancy, as shown in Figure 1. Enlarged lymph nodes surrounding the lesion were observed. Two attempts of CT guided needle biopsy were not diagnostic, containing mostly liver tissue with a small amount of abscess debris. MRI showed a high T1 signal in the suspected lesion, medial to the gallbladder. However, no obvious enhancement of the lesion was observed.
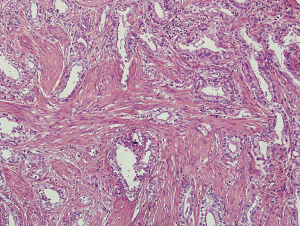
The patient underwent exploratory laparoscopy which was converted to a laparotomy, (due to complicated anatomy). A large cystic lesion, filled with blood, underneath segment 4 of the liver and near the gallbladder was witnessed. The tissue in the vicinity of the fundus of the gallbladder was sent for frozen section and was reported as positive for adenocarcinoma. Enlarged lymph nodes closest to the lesion were also infiltrated by adenocarcinoma on frozen section. In particular, a large lymph node situated between the duodenum, the pancreas and the distal CBD revealed to be vigorously infiltrated by adenocarcinoma. Cholecystectomy and excision of the lesion were performed. Pathologic findings demonstrated the cystic lesion to have a partial, thick smooth muscle coat and to be lined by neoplastic epithelium with biliary and squamous features (Figure 2), while the cyst wall itself was fibrous in nature. While adenosquamous carcinoma infiltrated the cyst wall, most of the tumor present outside of the gallbladder. Specifically, it was observed invading into a small area of the fundus of the gallbladder, connective tissue above the cystic duct and into the area of the hepatoduodenal ligament. The gallbladder mucosa in the area of invasive tumor was focally infiltrated by neoplastic glands, potentially infiltration of adenocarcinoma into the mucosa. The remainder of the gallbladder mucosa showed changes of chronic cholecystitis.
Immunohistochemistry staining of the tumor tested positive for CK7, MUC1 and focally positive for CK20, CDX-2 stained a few cells lining the inner surface of the lesion and MUC2 was essentially negative. The findings were consistent with a biliary profile. The pathological findings mandated a second laparotomy that was performed a week later, and a non-anatomical liver resection of segments 4 and 5, extensive lymph node dissection of the hepatoduodenal ligament, inter aortico-cave below the left renal vein and the celiac region, as well as the excision of residual periportal tumor with the distal CBD and a Roux-en-Y hepaticojejunostomy anastomosis were performed. The entire area was marked by clips for tracking during the course of future radiotherapy. Upon comprehensive review of the anatomic findings, radiologic imaging and pathology reports, our multi-disciplinary team concluded that the tumor was arising from a duplication cyst of the gallbladder.
The post-operative course was uneventful, and the patient was successfully discharged with follow-up adjuvant chemoradiation therapy. 18 months after her operation the patient is alive with no evidence of disease in her liver or abdomen. However, subsequent CXR, CT scan revealed diffused lung metastasis.
Discussion
Anatomical variations of the gallbladder are extremely rare with duplicate gallbladders reported in 1 per 12,000 cholecystectomies and 1 in 4,000 autopsies (1). Several anatomical variations of gallbladder duplication have been described (2), including bifid gallbladder, double gallbladders with two cystic ducts, as well as other very rare variations including duplication cyst of the gallbladder (3). Another relatively rare differential diagnosis is biliary choledochal cysts, which has an incidence of 1:1,000 newborns in Asia compared to 1:35,000–1:150,000 newborns in the US and Australia (4). Both gallbladder duplications and choledochal cysts are most often diagnosed before the age of ten, but may be present in later adulthood (3). Abdominal pain is the most frequent symptom of a duplicated gallbladder and choledochal cysts, with malignancy as a well-known complication of choledocal cysts. In a recent study of 5,780 patients undergoing resection of a choledocal cyst, Sastry et al. (4) reported an incidence for adenocarcinoma of 11.4% in adults with a peak in the 6th to 7th decade where the malignancy rate was 38%. Only 9 cases (0.42%) were seen before the age of 18. To the best of our knowledge adenocarcinoma arising in a duplicated gallbladder cyst has not been previously reported. A case report describing epithelial cyst of the gallbladder associated with adenocarcinoma has been reported by Matsumoto et al. (5), however the cyst was intramural. In our patient, adenocarcinoma was found arising in a cystic structure medial to the gallbladder, with no apparent anatomical communication with the gallbladder or biliary tree demonstrated by imaging studies or at surgery. Significantly, the wall of the cyst in part contained a thick smooth muscle coat and was lined by neoplastic biliary and squamous epithelium. Differential diagnosis for the lesion theoretically included: a type II choledocal cyst, severe hydrops of the gallbladder and a duplicate gallbladder. While smooth muscle may be variable presentation in a choledocal cyst, the presence of a thick, well defined smooth muscle coat in the cyst wall makes a choledocal cyst unlikely. In addition, given that the lesion was separate from the gallbladder, it was concluded that the cystic structure represented a duplicate gallbladder.
Conclusions
Duplicate gallbladder cyst is a rare anatomical finding, malignancy arising in it have not yet been reported, but should be considered and investigated as a possibility based on the clinical and radiologic findings.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Ozgen A, Akata D, Arat A, et al. Gallbladder duplication: imaging findings and differential considerations. Abdom Imaging 1999;24:285-8. [Crossref] [PubMed]
- Moore TC, Hurley AG. Congenital duplication of the gall bladder; review of the literature and report of an unusual symptomatic case. Surgery 1954;35:283-9. [PubMed]
- Kothari PR, Kumar T, Jiwane A, et al. Unusual features of gall bladder duplication cyst with review of the literature. Pediatr Surg Int 2005;21:552-4. [Crossref] [PubMed]
- Sastry AV, Abbadessa B, Wayne MG, et al. What is the incidence of biliary carcinoma in choledochal cysts, when do they develop, and how should it affect management? World J Surg 2015;39:487-92. [Crossref] [PubMed]
- Matsumoto M, Maruta M, Maeda K, et al. Epithelial cyst of the gallbladder associated with adenocarcinoma. J Hepatobiliary Pancreat Surg 2002;9:389-92. [Crossref] [PubMed]